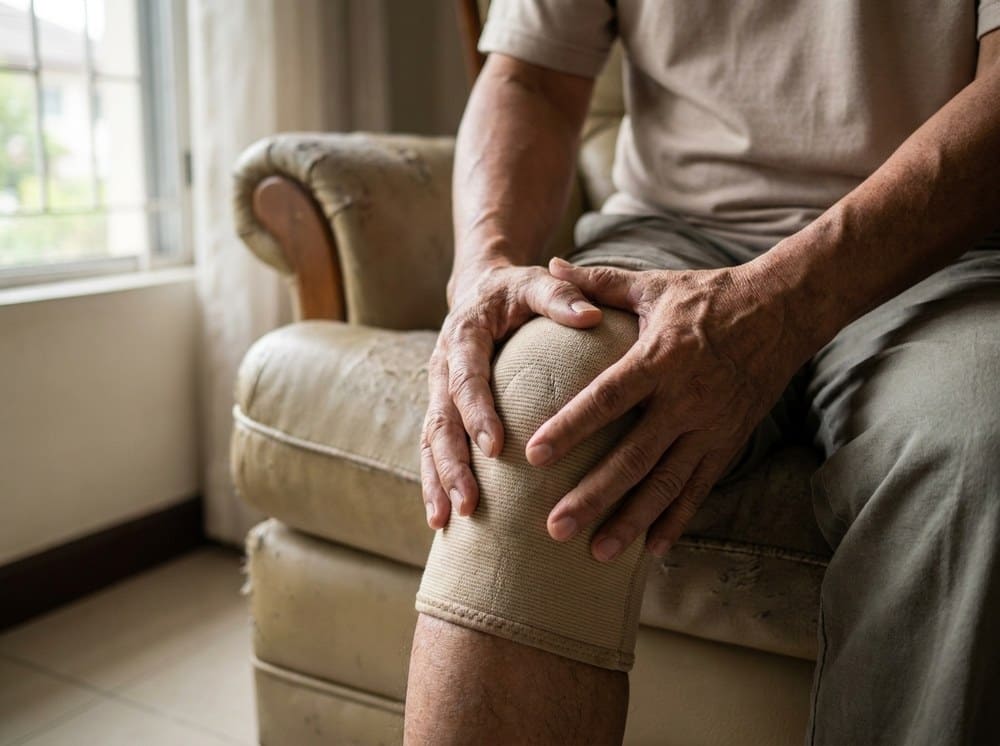
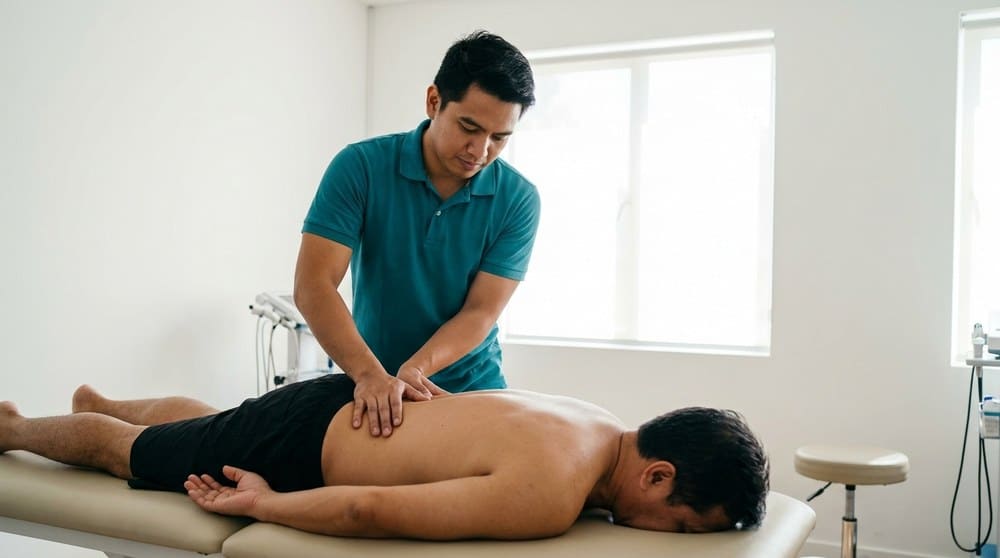
Every week, we meet patients who say some version of this: "I went to my GP three months ago, took the painkillers, and the pain came back." The painkiller worked. The problem did not go away because painkillers do not fix movement problems — they quiet them. Joint pain that comes back reliably after you stop medication is almost always a signal that the mechanics around the joint need attention, not just the chemistry inside it. That is where a physiotherapist fits in, and here is how to know when to make that call.
What a GP does well — and where the limits are
Your family doctor is fantastic at three things when it comes to joints: ruling out dangerous conditions (fracture, infection, autoimmune disease), prescribing short-term medication for flare-ups, and referring out when needed. That is real value. But a 15-minute GP appointment rarely allows for detailed movement analysis, manual therapy, or progressive exercise prescription — and those are exactly the tools that resolve the mechanical causes of most joint pain.
A licensed PT in the Philippines completes 5 years of university training plus board licensure through the PRC. Geriatric, sports, and orthopedic subspecialties extend that further. What we spend hours training for is watching, testing, and progressing human movement. That is the gap we fill.
Red flags that warrant professional attention
Some signs mean "see someone, and do not wait." If you tick any of these, book an assessment this week:
- Joint pain lasting more than 3 weeks despite rest
- Visible swelling, warmth, or redness around a joint
- Morning stiffness lasting more than 30 minutes
- Pain that wakes you up at night
- Noticeable loss of range of motion (you cannot fully bend or straighten the joint)
- A joint that gives way, buckles, or "locks" during activity
- Pain after a fall or obvious injury
- Spreading pain — starts in the knee, ends up in the hip or back
The last point deserves emphasis. Pain migrates because the body compensates. A sore knee leads to a hitched walk, which overloads the opposite hip, which then tightens the lower back. By the time the back hurts, most people have forgotten about the knee. This is the pattern we untangle every day.
Tip from our team
If you are about to book a GP visit for joint pain, ask one question: "Can you order an X-ray so I can also go straight to physiotherapy?" Most GPs will happily do both in one visit. This saves a round trip and speeds up getting to the right treatment by one to two weeks.
What a physiotherapist does that a GP cannot
Here is the practical list, not the textbook list:
1. Full biomechanical assessment
We watch you walk, sit, stand, squat, and reach. We test every joint above and below the painful one. We measure strength, range, and muscle control — and we give you a clear map of what is driving the pain, not just where you feel it.
2. Hands-on manual therapy
Joint mobilizations, soft-tissue release, trigger point work, and myofascial techniques. These directly reduce pain and restore movement in ways medication cannot. Most patients feel a noticeable difference after the first session.
3. Progressive exercise prescription
Generic "do some stretches" is useless for a stiff knee. What works is a specific, progressive loading program tailored to your exact joint, stage, and tolerance. We build it, supervise you through the early stages, and hand it off when you can run it yourself.
4. Education and pattern interruption
We teach you why your joint is behaving this way, what triggers flare-ups, and how to modify daily tasks — standing at the jeepney stop, sitting at your desk, carrying groceries up three flights when the elevator is out again. This knowledge is portable. Medication is not.
5. Coordination across specialties
If your symptoms suggest rheumatoid arthritis, we say so and refer. If they suggest a torn meniscus, we coordinate imaging and orthopedic consult. We are not trying to be everyone's only provider — we are trying to be your movement quarterback.
Honest observation after a decade in Makati: patients who see a PT in the first 6 weeks of joint pain recover roughly twice as fast as those who wait 6 months. The joint has not changed — the surrounding tissues have.
Navigating HMO referrals in the Philippines
Good news: in the Philippines, you do not legally need a GP referral to see a PT. Any PRC-licensed physiotherapist can assess and treat you directly. The HMO side is a bit more nuanced, though — here is what usually works:
Option A: Direct access with HMO session benefits. Some HMO plans include a set number of PT sessions per year without requiring GP referral. Ask your HMO coordinator or check your benefits booklet. Many Maxicare, Medicard, and Intellicare plans now include this.
Option B: GP referral + LOA. The most common pathway. Your GP writes a referral, the HMO issues a Letter of Authorization (LOA) specifying the number of sessions covered. The LOA lives for a fixed period (usually 30–60 days) and can often be renewed.
Option C: Self-pay the assessment, then decide. This is what a surprising number of our patients choose. A first assessment at MotionPath is affordable, and they use it to decide whether to pursue HMO-covered sessions or go private. No commitment, no paperwork on day one.
If you are confused about which option fits your situation, call us before booking. Five minutes on the phone with our admin team will save hours of back-and-forth. For broader context on the healthcare landscape, see our guide on understanding arthritis for Filipinos over 50.
What a first session actually looks like
A typical first visit at our Legazpi Village clinic takes 45 to 60 minutes. We start with your history — what you feel, when, for how long. We move through a physical assessment. We explain what we see in plain language, not jargon. By the end, you should leave with three things: a clear diagnosis, a realistic plan (how many sessions, over what time frame), and one or two starter exercises you can do at home that day.
No scare tactics, no vague "maintenance packages," no selling of supplements. If you do not need physiotherapy — if your pain will resolve with rest and adjusted habits — we tell you honestly. We would rather lose a session's revenue than waste your time.
The cost of waiting
People wait because waiting is free. It is not. Joints that go untreated for 6+ months develop compensations that are harder to reverse. Muscles weaken, ranges shorten, and what could have been a 4-session fix turns into a 10-session fix — or a surgical discussion.
If your joint has been talking to you for more than a month and your GP's painkillers are not finishing the conversation, it is probably time for a different specialist in the room. Whether it is us or another licensed PT, the sooner the better. For the specific case of knee and arthritic joints, our structured knee and arthritis care program is where most patients end up — HMO-supported, licensed, and focused on function rather than quick fixes.
 By Dr. Marianne Aquino
By Dr. Marianne Aquino